The neuro-ophthalmology department provides expert care for vision problems caused by neurological conditions, bridging the gap between eye health and brain function. We diagnose complex disorders such as optic neuritis, double vision, visual field loss, and cranial nerve palsies—using multimodal imaging and a multidisciplinary approach to protect both sight and neurological well-being.
Perimetry in stroke refers to the assessment of visual field defects in individuals who have suffered a stroke. A stroke can damage the brain's visual processing centers, leading to visual field defects, which can affect a person's daily life and independence.

Types of visual field defects in stroke:
Perimetry tests used to assess visual field defects in stroke:
Importance of perimetry in stroke:
Treatment options for visual field defects in stroke:
Non-arteritic anterior ischemic optic neuropathy (NAION) is a condition where the blood flow to the optic nerve is suddenly interrupted, causing damage to the nerve and potentially leading to permanent vision loss.
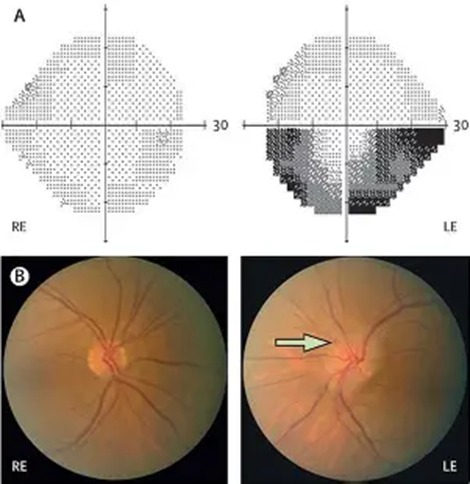
Causes:
Symptoms:
Diagnosis is made by clinical examination, visual field testing, optical coherence tomography (OCT) and fluorescein angiography
Treatment:
Prognosis:
It's essential to seek medical attention immediately if symptoms occur, as prompt treatment may help reduce the risk of further vision loss.
Idiopathic intracranial hypertension (IIH), also known as pseudotumor cerebri, is a condition characterized by increased pressure within the skull without any apparent cause. The condition is often associated with obesity, and women of childbearing age are more commonly affected.
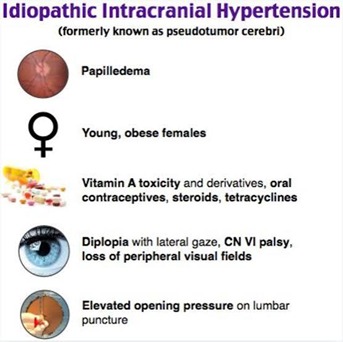
Symptoms:
Diagnosis:
Treatment:
Complications:
It's essential to seek medical attention if symptoms persist or worsen over time. Prompt treatment can help alleviate symptoms, prevent complications, and improve quality of life.
Optic neuritis is an inflammatory condition that affects the optic nerve, which carries visual information from the eye to the brain. It can cause vision loss, pain, and other symptoms.
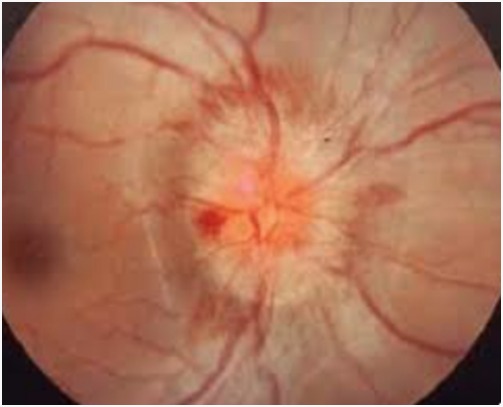
Symptoms:
Causes:
Diagnosis:
Treatment:
Prognosis:
It's essential to seek medical attention promptly if symptoms occur, as timely treatment can improve outcomes and reduce the risk of complications.

DO, FICO
stethoscope_arrow Neuro Ophthalmology, General Ophthalmology
event_available OP Days:
Monday,Tuesday,Wednesday,Thursday,Friday,Saturday