Our vitreoretina services offer care for conditions affecting the retina and vitreous, which are critical to maintaining central vision. We treat a wide range of disorders including diabetic retinopathy, age-related macular degeneration (AMD), retinal detachment, macular holes, vitreomacular traction, retinal vein occlusion, using cutting-edge diagnostics and treatments to preserve sight and improve outcomes.
Diabetic retinopathy (DR) is a complication of diabetes that affects the blood vessels in the retina, leading to vision impairment and potentially blindness. It occurs when high blood sugar levels damage the blood vessels, causing them to leak, swell, or grow abnormally.

There are two main stages of DR:
In the early stages of diabetic retinopathy, patients usually have no symptoms. Hence it is crucial that every diabetic should have a retinal examination at least once a year even if they are otherwise healthy.
Risk factors for DR include duration of diabetes, poor blood sugar control, hypertension, and hyperlipidemia. Early detection and treatment, including laser photocoagulation and anti-vascular endothelial growth factor (VEGF) injections, can help prevent vision loss and slow disease progression.
Anti-Vascular Endothelial Growth Factor (VEGF) injections are a treatment for various eye conditions, including:
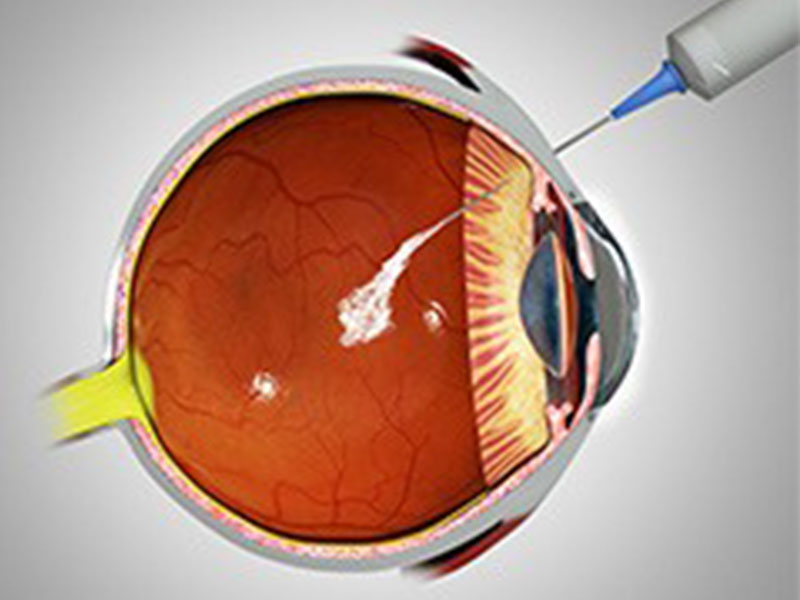
These injections work by blocking the action of VEGF, a protein that promotes the growth of new, fragile blood vessels in the eye. By inhibiting VEGF, the injections help to:
The most commonly used anti-VEGF medications are:
Treatment typically involves a series of injections, with the frequency and number of injections varying depending on the condition being treated and the individual’s response.
Treatment for diabetic retinopathy (DR) aims to slow disease progression, reduce vision loss, and improve quality of life. The goal is to prevent complications, such as blindness, and address related conditions, like diabetic macular edema (DME).

Treatment options include:
It's essential to work closely with an eye doctor to determine the best treatment plan, as it may vary depending on the severity and type of DR, as well as individual patient factors. Regular follow-up appointments and monitoring are crucial to prevent vision loss and address any complications that may arise.
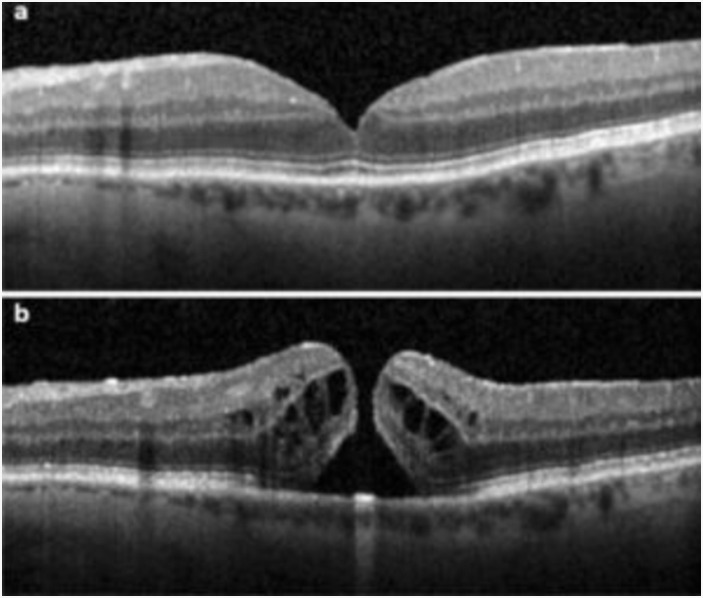
Macular hole surgery, also known as vitrectomy with membrane peeling, is a surgical procedure used to treat a macular hole, a small break in the macula, the part of the retina responsible for central vision. The goal of surgery is to remove the vitreous gel, peel the epiretinal membrane and allow the macula to heal and the hole to close, improving vision.
Patient is required to maintain a face-down position for several days to help the hole close.
Retinal detachment surgery aims to reattach the retina to the back of the eye. Surgical options include:

Success rates are high, with 80-90% of patients achieving retinal reattachment.
Post-operative care:
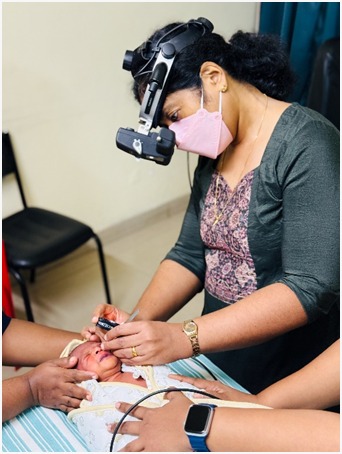
Retinopathy of Prematurity (ROP) is an eye disease that can happen in babies who are premature or who weigh less than 1500 grams at birth. ROP happens when abnormal blood vessels grow in the retina. Some babies with ROP have mild cases and get better without treatment. But some babies need treatment to protect their vision and prevent blindness. There are different stages of ROP. Doctors use these stages to keep track of how serious the disease is.
It is important to make sure that the follow up exams are on schedule. There are no signs of ROP. If your baby is at risk of ROP, he/she will need a dilated exam, a few weeks after they are born. During the exam the eye doctor will dilate the pupils and check for growth of the retinal blood vessels.
Babies in stage 1 and 2 usually get better without treatment while babies in stage 3, 4 and 5 will need some sort of treatment in the form of laser, injections or surgery. It is also possible for babies in any stage to get worse quickly and need treatment. So it is important to review with your doctor at the correct time to prevent chances of blindness.

D.O., D.N.B., ICO, FMRF, FRCS(GLASG)
stethoscope_arrow Vitreo Retina, General Ophthalmology
event_available OP Days:
Monday,Wednesday,Thursday,Friday

D.O., D.N.B., MS, FRCS
stethoscope_arrow Vitreo Retina, Cataract & IOL Services, General Ophthalmology
event_available OP Days:
Thursday,Saturday

MS, FVRS
stethoscope_arrow Vitreo Retina, General Ophthalmology
event_available OP Days:
Monday,Tuesday,Wednesday,Thursday,Friday,Saturday